You can change the conversation. Chip in to rabble’s donation drive today!
Injection drug users often report feeling completely consumed by their addiction, trapped in a cycle of drug use, crime and incarceration. People who struggle with addictions are more likely to have suffered challenging experiences such as poverty, physical or psychological traumas or a have a history of psychiatric illnesses and are also more likely to come to the attention of the criminal justice system, particularly if their drugs of choice are illegal.
With this interest in addiction treatment, prison health care and advocacy on behalf of marginalized groups, on January 23 On Point: Making Prison Needle & Syringe Programs Work in Canada was held.
What is harm reduction?
The addiction medicine community has long recognized that punishing people for using drugs is ineffective. Addiction is a complex and frequently relapsing disorder involving a multitude of factors and punishment only serves to criminalize rather than treat their disorder.
For example, Methadone maintenance programs had their genesis in the 1960s, when physicians Vincent Dole and Marie Nyswander, who were treating heroin addiction in New York City, observed a cycle of repeat incarceration. Their patients would undergo involuntary detoxification in jail, only to resume heroin use upon release and eventually die of their addiction.
Among Canadian prison populations, surveys performed by the Correctional Service of Canada identify that by 2002 as many as 70 percent suffer from a substance use disorder.
The Public Health Agency of Canada identifies that “the sharing of injection equipment is … a major risk behaviour frequently practiced within correctional facilities.” Given that inmates in Canadian prisons have a rate of HIV and Hepatitis C ten and 30 times higher than the general population, respectively, reducing these infections in prisons seems essential for the health of inmates and the communities to which they could return.
Many jurisdictions have recognized the reality of drug use in prisons and have instituted needle and syringe exchange programs. These programs come out of the harm reduction model of addiction treatment, a non-judgemental ethos that encourages an eventual cessation of dysfunctional drug use while tolerating relapses in an effort to reduce harmful behaviours. Germany, Switzerland, Spain, Moldova, Kyrgystan, Iran, Armenia, Ukraine and Belarus have successfully adopted needle and syringe exchange programs in prisons.
Despite these successes, the Canadian government continues to support these programs only outside of correctional facilities.
Why is harm reduction in Canadians prisons necessary?
Correctional Service of Canada reports that aboriginal people comprise four per cent of the population in Canada but 23 per cent of prison inmates, and they are more likely to suffer from HIV/AIDS and Hepatitis C infections.
Mi’kmaq prison activist Julie Thomas, the program manager of Healing Our Nations, says that most inmates don’t stay in prison for life, but are eventually released and return to their communities. Since incarceration is itself a risk factor for contracting HIV and Hepatitis C, the over-representation of aboriginal inmates in prison may result in disproportionately more HIV and Hepatitis C in aboriginal communities compared with the Canadian population as a whole.
“More harm reduction is needed inside,” says Thomas, describing the unsafe conditions in prisons that promote the transmission of disease. Inmates reported injecting drugs for the first time in prison because they were bored or wanted to “fit in” and that as many as 20 to 30 people have shared one syringe, dulling it to the thickness of a ballpoint pen. And also, of inmates lacking a syringe and instead using razors to open their veins.
Canadian prisons have provided bleach kits since 1996, and though bleach erradicates HIV, it doesn’t kill Hepatitis C. Inmates have said that fetching a bleach kit can trigger a cell search and that the bleach kits are in poor condition, lacking bleach or rusted. Thomas met inmates who claimed to have contracted HIV inside prison usually from needle-sharing, but also through fights where blood was spilled and punching bags splattered with blood. Female inmates have said they contracted HIV from sharing dildos.
Thomas’ observations were corroborated by the others.
Dr. Ruth Elwood Martin, who worked as a physician at the Burnaby Correctional Centre, describes finding more women with disease, such as previously undiagnosed HIV and hepatitis C infections and untreated cervical cancer, than she had ever encountered in her career. Martin estimates that nearly all the women under her care used street drugs before they went to jail.
A survey performed at her facility found that 21 per cent of incarcerated women reported using needles to inject drugs. Eighty-six per cent of injection drug users said they shared needles, but the vast majority of injection drug users, 90 per cent, will use bleach kits if they are available.
Bleach kits are not enough, says Sandra Ka Hon Chu, a lawyer who launched a lawsuit in 2012 to force the Canadian government to bring needle exchange programs into penitentiaries. Ka Hon Chu outlines the government’s objections as the availability of injection equipment will: (1) promote drug use, (2) increase violence in institutions, and (3) not work in Canada because the prison system is unique.
In fact, offering needle exchange programs decreases needle sharing, has no influence on drug use and there has not been one single case of a syringe being used as a weapon since 1992, the year needle exchange programs were first introduced. In prisons with needle exchange programs, staff have said they actually feel safer because they don’t worry about coming across hidden needles that have been used by potentially dozens of people when conducting cell searches.
Dr. Daniela De Santis, a physician at Hindlebank Prison in Switzerland, which has had needle exchange programs since 1994, says “if one HIV infection is prevented, my salary is paid for two years.”
The evidence in favour of harm reduction programs is too overwhelming to ignore. The Canadian government needs to implement a harm reduction program in prisons and allow some of our most vulnerable citizens to help themselves.
Like this article? Chip in to keep stories like these coming!
Denise Denning is a pharmacist who trained in addiction treatment at the Addiction Research Foundation (now the Centre for Addiction and Mental Health) and has worked for the past 17 years primarily dispensing methadone to people both in and out of jail.
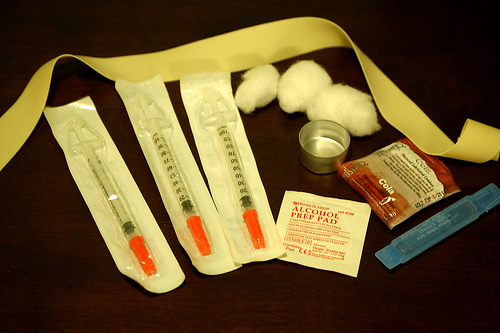
Photo: flickr/Todd Huffman